Nevada health clinics fear vulnerable patients will be harmed if federal funding dries up

By Jackie Valley and Megan Messerly
https://thenevadaindependent.com
After staffers saw their morning patients at Hope Christian Health Center, they began to prepare hot dogs, hamburgers and fixings for a miniature potluck.
Doug Self, the center’s chief executive officer, asked a patient in the clinic if she wanted to join. The woman immediately started crying.
“I would love to if you let me,” Self recalls her telling him. “I haven’t eaten in a couple days.”
Moments like that remind Self he made the right decision. The former hospital administrator moved to Las Vegas a few years ago with dreams of entering the classroom, but during his first semester as a seventh-grade math teacher, his background came calling: Hope Christian Health Center had just received designation as a federally qualified health center, and it needed a seasoned administrator.
Self, who had volunteered to be on the health center’s board shortly after moving here, didn’t want to see the fledgling operation fail. So he traded the classroom for the clinic setting again and assumed the role of CEO.
“I just feel much more rewarded now in doing this job than I ever have my entire life,” he said. “Whenever we talk about health care on a national and state level, we forget about a lot of people left behind.”
He’s referring to the center’s patient population: 50 percent are on Medicaid, 25 percent are uninsured and the remaining 25 percent have some form of private insurance. The options for those without insurance or on Medicaid are limited at best, given the small number of physicians willing to see either type of patient.
Hope Christian Health Center sought to fill that void. The center served 60 patients in June 2015 and swelled to seeing 440 patients in May this year.
The growth in patient volume triggered a search for a larger space in North Las Vegas. They found the perfect location — a 5,000-square-foot space in a new plaza near Martin Luther King Boulevard and Craig Road — and began renovations.
But funding uncertainty for federally qualified health centers threatens to disrupt the organization’s expansion plan.
Nevada’s federally qualified health centers
So-called federally qualified health centers are federally funded nonprofit health centers or clinics serving medically underserved areas and populations that provide services to patients regardless of their ability to pay. FQHCs qualify for funding under Section 330 of the Public Health Service Act and receive enhanced reimbursement rates for Medicare and Medicaid patients.
Nevada’s six federally qualified health centers provide services at 33 sites across the state, many of them clustered around the Las Vegas and Reno metropolitan areas but a handful scattered across the state’s rural and frontier counties. Nevada Health Centers, the state’s largest federally qualified health center operating 16 sites across the state, has facilities in Elko, Eureka, Crescent Valley, Carlin, Wendover, Jackpot, Austin, Amargosa Valley, Lockwood and Virginia City.
But the future of federally qualified health centers hangs in the balance, with Congress pushing up against a Sept. 30 deadline to extend funding for the centers. Both of Nevada’s senators, Democrat Catherine Cortez Masto and Republican Dean Heller, sent a letter this week along with 68 other senators to Republican Sen. Lamar Alexander and Democratic Sen. Patty Murray, the chairman and ranking member on the Senate Committee on Health, Education, Labor and Pensions, respectively, urging a “swift resolution” to the funding cliff health centers face.
“Community health centers serve a critical role in communities throughout the United States and are important safety net providers,” the senators wrote. “If Congress allows the Community Health Centers Fund (CHCF) to lapse, it would immediately threaten patient access to the cost-effective primary and preventive care health centers provide.”
Last week, a bipartisan group in the House introduced a bill to extend community health center funding for five years, with increases to account for more demand and to bolster services in national priority areas. But there’s been no movement on the legislation since it was introduced, and it is unclear whether it would be the legislative vehicle to move the funding for the health centers forward.
Not only are federally qualified health centers an integral part of Nevada’s health-care safety net in the urban areas, in rural Nevada, the centers are often the only health clinic around for miles and the primary care provider for people regardless of their insurance status. Facing the looming fiscal cliff, the rural community health centers are reiterating their commitment to finding new resources should the federal government not renew the funds while continuing to provide the same level of service at their clinics.
“Our rural people, they just have so much to worry about accessing health care as it is. Is their provider going to stay there? Are we going to continue being open the hours they’re open?” said Lisa Dettling, vice president of mission strategy for Nevada Health Centers. “I’d hate to worry them. I want to assure them that we will continue to provide services.”
But Steven Messinger, policy manager for the Nevada Primary Care Association, said he fears rural clinics could be the hardest hit because they often operate at a loss and are subsidized by urban clinics. On top of that, they’re difficult to staff.
“My concern is that they would be the first to go,” he said.
The funding game
A little more than a quarter of Nevada Health Centers’ budget is funded through federal dollars, with about 50 percent coming from patient revenue and a little less than 25 percent from community partnerships, where a city may pay a flat fee every year or month to support a health center, or other grant funding. Dettling said there is no contingency plan in place if the federal funding is cut — whether the organization would have to reduce services, reduce clinics or reduce staff — but their hope is that they would quickly find adjustments and opportunities to make it work.
“I think the message (our CEO) has been very clear with our whole organization is, ‘Look, we’ve been here 40 years in Nevada. We’ve been through highs and lows and we have figured it out every time,’” Dettling said.
Last year, federally qualified health centers served 89,000 people in Nevada, Messinger said. Ninety-five percent of those people live at 200 percent of the federal poverty level, and two-thirds are ethnic or racial minorities.
Nevada’s system of community health centers isn’t as robust as some other states’, but it has grown in recent years, buoyed by federal-funding increases, Messinger said. Nevada received a 51 percent surge in federal funding from 2014 to 2016, bringing last year’s amount up to $18.4 million.
About 70 percent of that funding is at risk if Congress doesn’t act on or before Sept. 30, Messinger said. The other 30 percent is part of the government’s normal budgeting process. President Donald Trump recently signed a continuing resolution that keeps the government funded into December.
Officials from the Health Resources & Services Administration said the agency will provide “partial continuation awards” within available funds.
“Beyond that we cannot speculate about future funding issues,” HRSA spokesman Scott Kodish wrote in an email.
The Community Health Alliance, which operates six centers in Reno and Sparks, estimates that federal funds account for between 15 and 20 percent of its annual operating budget. Those $4 million in funds help the clinic serve uninsured patients, including the homeless population in Northern Nevada.
CEO Chuck Duarte said the organization has been “squirreling away” money by creating cash reserves so that they wouldn’t have to implement immediate cuts in services if the federal funding is not reauthorized.
“Reducing hours, closing facilities, ending programs — I don’t want to do an across-the-board reduction, because that affects everybody, but more targeted and direct,” Duarte said. “Rather than robbing Peter to pay Paul, looking at it more directly and what it might do to patients.”
Duarte is also concerned about the reauthorization of National Health Services Corps funding, which goes hand-in-hand with the health center funding. The NHSC helps support providers who choose to work in underserved areas, such as offering a loan repayment program that gives providers tax-free loan repayment assistance.
“The ability to have their homes repaid through working for a community health center like ours — it’s one of our biggest recruiting tools,” said Duarte, who estimates about four out of five of the center’s licensed clinical professionals have benefitted from the program either previously or on an ongoing basis.
Traditionally, community health centers have been a bipartisan issue because they exist in most congressional districts, but Messinger fears the nation’s unpredictable political environment paired with other unexpected funding needs, such as hurricane relief, could spell trouble this year.
“There’s a lot going on besides the political climate that just makes everything tough,” he said.
The waiting game
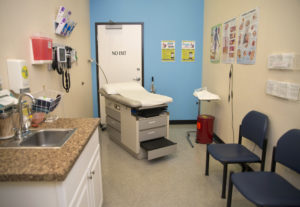
Uninstalled cabinets sat in the lobby of Hope Christian Health Center’s new space this week, waiting to be brought to their final resting place. Boxes lined nearby rooms and hallways. And an empty desk occupied an office.
But if you looked closely enough, you could see hints of a clinic taking shape: an exam table in a patient room, complete with a pillow on top.
The rest should be in place by Oct. 3. That’s when Self intends to open the new Hope Christian Health Center, which is days after the looming Sept. 30 deadline for reauthorization of federal funding.

“I’m worried about it,” he said. “It’s not so much that I’m worried the funding won’t happen. I’m worried when the funding will happen.”
Federal funding makes up 60 percent of the health center’s monthly budget, meaning it would have to “greatly reduce” the amount of health care provided to patients at a time when it planned to be expanding those services, Self said. Staff furloughs would be another possibility if the federal funding dries up.
The center’s staff includes a full-time doctor and two nurse practitioners as well as some clerical positions. The medical staff treat patients of all ages whose needs range from general check-ups to monitoring of complex medical issues such as high-blood pressure and diabetes.
“It’s such a hard thing to see a huge demand for need and then be worried about your funding and possibly not being able to provide for that need,” he said.




